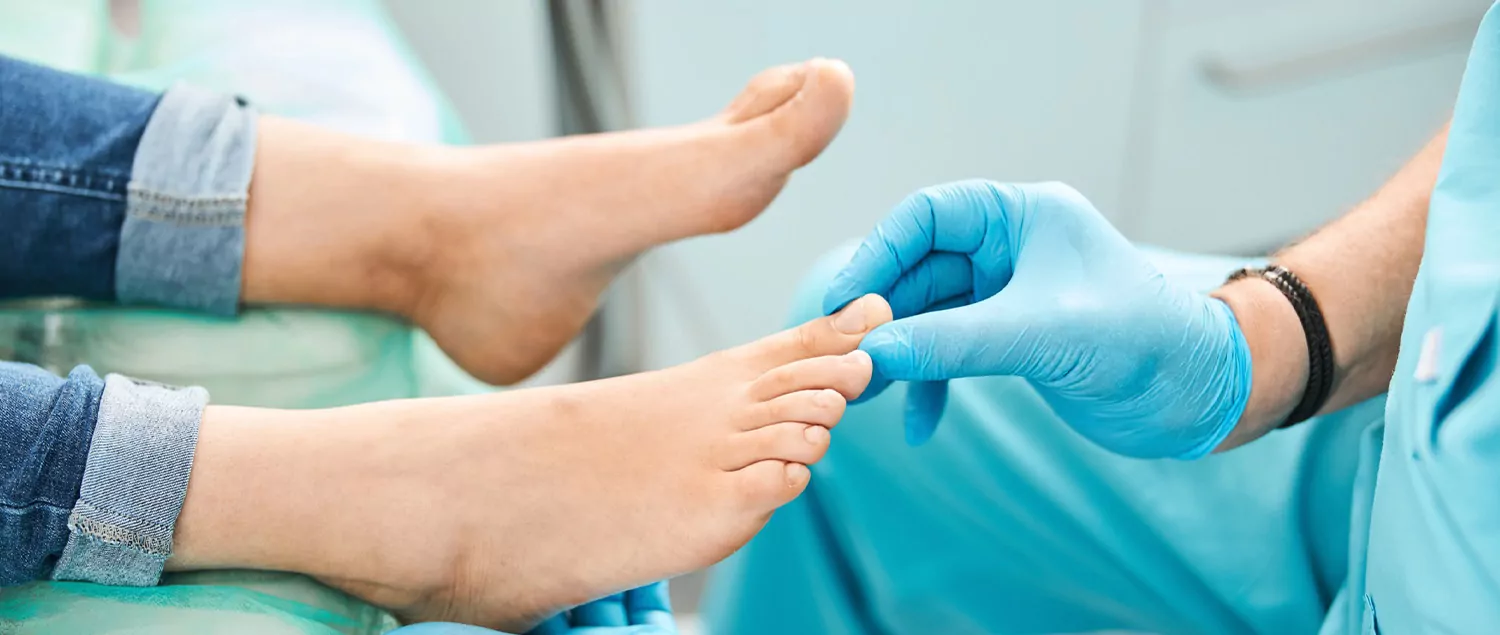
What is Diabetic Foot? What are the Symptoms?
Diabetic foot, also known as diabetes, is a condition in which high blood sugar causes damage to nerves and vessels. It can manifest itself as loss of sensation in the feet, numbness, tingling. In some cases, the patient may be injured due to reduced sensation and infections may occur. Since wounds take longer to heal than in a healthy person, the damage can be greater. In cases where there is no intervention or intervention is delayed, gangrene and amputation may occur.
Diabetes is seen in two different forms: type 1, where insulin is not produced, and type 2, where insulin is produced but not enough to lower blood sugar. These types of diabetes differ in their occurrence but result in high blood sugar. Untreated or inadequate treatment can lead to undesirable consequences such as cataracts, diabetic neuropathy and diabetic foot.
What is Diabetic Foot?
Diabetic foot is a problem that can extend to ulcers, loss of sensation and gangrene in patients with high blood sugar levels.
Neuropathy, which is seen in approximately 60% of diabetic patients, can manifest itself with different factors such as fungi, calluses, ulcer formations. Due to the long-term effects of high blood sugar, the patient has reduced blood circulation and a lowered immune system. The body is vulnerable to recurrent wounds and infections. This makes it difficult to treat these patients in whom healing is also slow. As the stages of diabetic foot progress, a condition known as Charcot’s foot or wobbly foot, in which the foot is not fully controlled and differentiated tissues are seen in terms of color and appearance, may occur.
Diabetes is a disease that needs to be kept under constant control. Treatment may include medications, surgical procedures, as well as life changes such as dietary modification and encouraging the patient to exercise. It is important to seek expert advice when necessary through medical examinations and remote health services. Delay or absence of treatment can lead to destruction of other organs in addition to the diabetic foot problem.
What are the Causes of Diabetic Foot?
A multi-layered mechanism operates in the formation of diabetic foot. To answer the question “How does a diabetic foot wound start?”, the wounds start and heal as small wounds in people who have had diabetes for a long time. Over time, nerve damage to the feet delays the recognition of injuries and blows to the feet in the patient’s daily life. Foot deformities such as calluses may occur in patients whose blood sugar is not kept at low levels. Factors such as not choosing appropriate footwear and walking barefoot can also increase the risk of injury.
Failure to keep the feet clean enough, combined with dry skin problems, paves the way for injuries. Blood flow in the feet and legs is reduced due to peripheral arterial disease caused by diabetes. This slows the healing of wounds. Wounds that heal late become vulnerable to fungal and bacterial infections. The answer to the question “When is the diabetic foot amputated?” is closely related to the mechanism of the diabetic foot. Amputation may be preferred to prevent the foot from affecting vital activities as nerve damage increases over time.
Diabetic Foot Risk Factors
Although the main cause of diabetic foot problems is high blood sugar, there are other reasons that increase the risk of their occurrence. Diabetic foot development is seen in patients who have been suffering from diabetes for many years and whose blood sugar levels remain at high levels. In overweight patients, the risk of diabetic neuropathy and diabetic ulcers increases as the disease has a greater impact on the nerves. It is more common in people over 40 who also have comorbidities such as high blood pressure and high cholesterol, with problems such as reduced blood circulation.
People with flat feet may develop wounds on more risky parts of the sole of the foot, as the pressure on a point in the foot will be greater. Factors such as smoking and sedentary lifestyles that lead to deterioration in general health increase the incidence of such problems. In order to minimize the risk of diabetic foot formation, it is very important for the patient to try to keep blood sugar values in balance, and to try to prevent blood flow and basic problems in the body with healthy nutrition and sports activities. Continuous cleaning and care of the feet can prevent the worsening of findings such as wounds and infections even if this type of problem occurs.
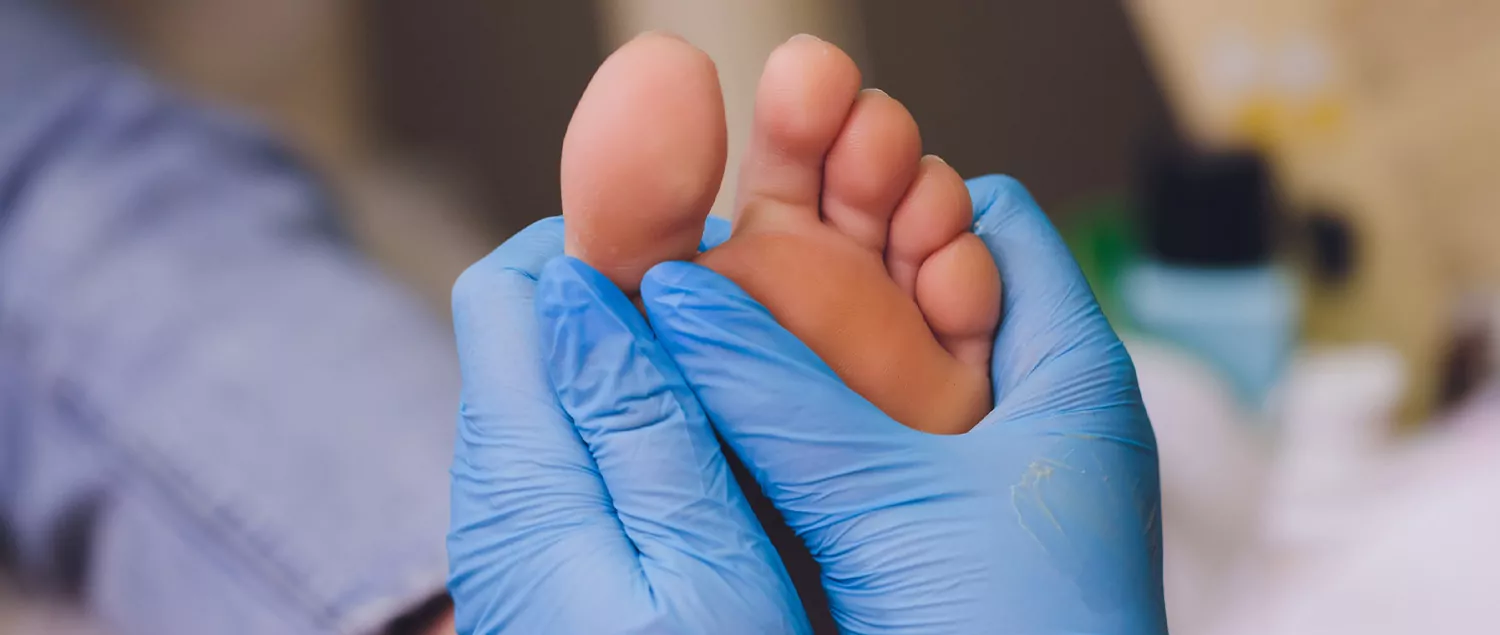
What are the Complications and Symptoms of Diabetic Foot?
There are some symptoms that indicate the occurrence of diabetic feet and can help the patient to recognize the condition. Symptoms of diabetic foot ulcers can be listed as follows:
- Abnormal changes in skin color
- Changes in skin temperature
- Swelling of the feet and ankles
- Pain in the legs and feet
- Frequent bleeding
- The presence of open wounds on the feet that take a long time to heal and recur with recurrent discharge
- Ingrown toenails and fungal infections
- Calluses and skin thickening
- Dryness in the feet, especially cracks in the heel
- Unbearable foot odor that is different from the usual
Problems called diabetic foot occur gradually. First of all, numbness and tingling in the feet appear. In the early stages, unnoticeable wounds may develop and heal. As a long-term effect of high blood sugar, wound healing slows down and infections occur in unnoticed open wounds. Infections are harder to heal because diabetes slows blood flow and lowers immunity. Untreated infections and increased cell death reduce blood supply to the foot. Complications known as gangrene, in which tissues are permanently damaged, can occur. After this stage, there may be no solution other than amputation of the diabetic foot.
How to Treat Diabetic Foot?
For diabetic foot treatment, it is very important to detect the problem in the early stages. In the presence of differential symptoms such as cold feet, one foot showing a different temperature than the other, inflammatory formations, some tests are performed on the systemic damage of diabetes. Whether the treatment will be outpatient or inpatient is decided based on variables such as the patient’s condition and the availability of caregivers.
The size of the infections and the causative bacteria are analyzed to decide on the right antibiotic and treatment is started. The next step involves focusing on problems with blood circulation. Revascularization, the process of opening vascular blockages with applications such as angioplasty and managing blood flow is applied to the patient. In this way, both the delivery of antibiotics to the area and the re-bleeding of the tissue can be targeted.
Treating and removing calluses and thickenings on the feet is essential to prevent recurrence of infections.
Wound closure materials and various care products can be preferred for non-healing and open wounds. In cases such as Charcot’s foot, which limits the movement of the foot, efforts are made to increase the movement capacity of the foot by using support equipment. By choosing orthopedic shoes suitable for the patient, the pressure on the wounds can be reduced and the factors that may cause new wounds to form can be eliminated.
After that, the process continues by following the treatment and the doctor’s recommendations and applying wound care. The question “Which doctor treats diabetic foot ulcers?” is also important for patients to determine the path they will follow for treatment. Doctors with various specialties such as infection specialist, cardiovascular surgeon, orthopedist can work in coordination for treatment. In the post-treatment process remote healthcare help from organizations can be effective in preventing recurrence of wounds.
How to Care and Dress Diabetic Foot at Home?
In addition to drug treatments, some methods to be applied at home before and after diabetic foot occurs can help prevent the development and progression of the disease. Some of the foot care suggestions that can be applied at home are as follows:
- It is important to check the feet regularly, especially by patients who have suffered from high blood sugar for many years. The earlier any changes, wounds or infections can be detected, the easier it is to intervene.
- Washing the feet with warm water every day is the right choice whether there is a wound or not. It can be considered the first step to prevent fungus and infections that may occur in the feet. Drying and moisturizing the feet after washing helps to heal wounds and cracks. Powder can be applied between the fingers and on the curved areas to prevent them from staying damp.
- Toenails should be trimmed regularly and filed correctly. Ingrown toenails can lead to sores and walking difficulties. For this reason, it should be prevented with correct pedicure applications.
- Calluses on the feet should be cleaned to prevent injury and infections. However, since this process involves procedures such as cutting the skin, it should be applied under the supervision of a doctor. Self-administered treatments may cause open wounds.
- Diabetic foot wound dressing should be done as recommended by the doctor and nurse. These directives usually include cleansing, drying, moisturizing and administration of antibiotic preparations.
- It is possible that the patient does not want to wear products such as slippers and shoes due to swelling in the feet. However, barefoot walking should be avoided to prevent injuries and thickening of the skin under the feet.
- Feet should be protected from cold and heat. Sunscreen should be applied to prevent burns when wearing open slippers in hot times, and heat-insulated shoes should be preferred in cold times.
- Socks and shoes that squeeze and disturb the feet should not be preferred, and the feet should be made comfortable.
- Maintaining blood flow in the feet is important to prevent loss of sensation. Appropriate sports and exercises can be effective both for the protection of general health and for accelerating blood flow. It may also be preferable as a precaution not to swing the feet from the seat during rest, but to extend them by placing a pillow under them.
- Even if your doctor forgets during routine examinations, reminding them to perform a foot examination can be effective for early diagnosis and rapid intervention.
In addition to such measures, regular blood sugar checks, a lower sugar content in the diet and regular doctor visits can be effective in preventing complications caused by diabetes. Health institutions that provide online doctor examination services can help in this process.